Adult soft tissue sarcoma is a disease in which cancer cells form in the soft tissues of the body. Soft tissues of the body include muscles, tendons, fat, blood vessels, lymph vessels, nerves and tissues around the joints. Adult soft tissue sarcoma is most commonly found in the head, neck, arms, legs and abdomen. Adult soft tissue sarcoma is diagnosed with a biopsy.

- Incisional biopsy : The removal of part of a lump or a sample of tissue.
- Core biopsy : The removal of tissue using a wide needle.
- Excisional biopsy : The removal of an entire lump or area of tissue that doesn’t look normal.
The treatment of soft tissue varies from case to case however the following are the most common treatments. After a biopsy, surgery is typically the first and main treatment for soft-tissue sarcoma that is small and located in only one area. Surgical oncologists and orthopedic oncologists are doctors who specialize in treating STS using surgery.
The surgeon’s goal is to remove the tumor and enough normal tissue surrounding it to obtain a clean margin around the tumor. A “clean margin” means there are no tumor cells visible at the borders of the surgical specimen. This is currently the best method available to ensure that there are no tumor cells left in the area from which the tumor was removed. Small low-grade sarcomas can usually be effectively removed by surgery alone. Those that are high grade and larger than 2 inches (5 cm) are often treated with a combination of surgery and radiation therapy. Radiation therapy or chemotherapy may be used before surgery to shrink the tumor and make removal easier. They also may be used during and after surgery to destroy any remaining cancer cells.
Rarely, for patients with a very large tumor involving the major nerves and blood vessels of the arm or leg, surgical removal of the limb, called amputation, is necessary to control the tumor. This can also be necessary if the tumor grows back in the arm or leg after surgery, radiation therapy, and/or chemotherapy have been completed. It’s important to remember that the operation that results in the most useful and strongest limb may be different from the one that gives the most normal appearance. If amputation is needed, rehabilitation, including physical therapy, can help maximize physical function. Rehabilitation can also help a person cope with the social and emotional effects of losing a limb.
My Surgery Experience
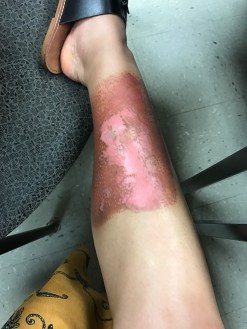
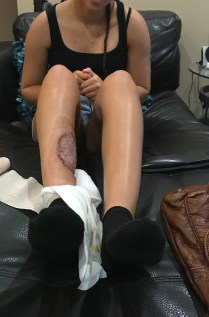
After my six week radiation therapy treatment, I was scheduled a month later for the cancer removal surgery. My cancer treatment plan was to shrink and remove the tumor with radiation as much as possible and then remove the tumor, as well as 2-3 cm margin around the tumor. This was to make sure that all margins were clear and cancer free. The area was checked by the pathologist upon removal. I was left with a deep hole in my shin that exposed my lower calf and shin.
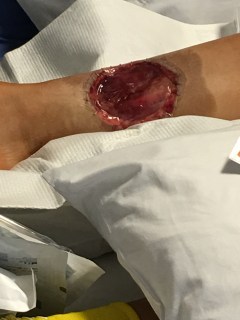
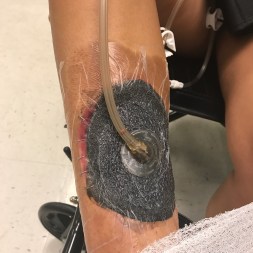
The hole in my leg was filled with a sponge and pump called a wound vac. A wound vac is the Vacuum Assisted Closure (VAC) device is used to facilitate wound healing by converting an open wound to a closed wound. VAC consists of an evacuation tube embedded in a polyurethane foam dressing. After the foam dressing is placed in the wound bed and sealed by an occlusive dressing, the tube is attached to a vacuum unit. The application of negative pressure causes the foam to collapse resulting in removal of excess fluids; increased blood flow and decreased bacterial colonization; granulation tissue formation; and wound closure. The wound VAC was worn for two weeks.
The next step and second surgery to become cancer free was a muscular flap and skin graft closure procedure. Flap surgery is a technique in plastic and reconstructive surgery where any type of tissue is lifted from a donor site and moved to a recipient site with an intact blood supply. This is similar to but different from a graft, which does not have an intact blood supply and therefore relies on growth of new blood vessels. In my case, my soleus muscle was taken and pulled across the hole and stapled in.

The surgeon then took skin from my hip/upper thigh and placed it over the muscle.
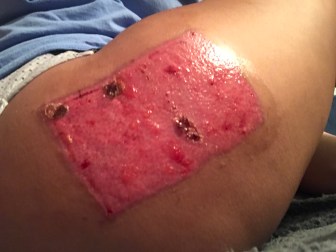
After having the surgery, I have to change the wound area everyday to make sure the area is healing properly as to make sure there is no infection. Changing the area is difficult at first and takes getting used to. I am currently in physical therapy to regain use of my leg and motion in the calf and ankle.
.